
David Erlinge
Professor of Cardiology
Wallenberg Clinical Scholar 2015
Institution:
Lund University
Research field:
Treatment and prevention of heart attacks


Wallenberg Clinical Scholar 2015
Institution:
Lund University
Research field:
Treatment and prevention of heart attacks
Professor Erlinge begins the interview on his feet. In 15 minutes a suspected heart attack patient is due to arrive by ambulance.
Alongside his full-time role as a researcher, Erlinge works 30 percent of full-time at the clinic. This is one of his clinic weeks, and when the patient has been prepped by the nurses it is his job to examine the coronary arteries, and open any that are blocked.
“As a clinician I go to work and deal with whatever comes up. In research, I draw up a plan for several years ahead. The roles are very different, and when I’ve been doing a lot of one thing, I long to get down to the other,” he says.
Clinical research involves patients; preclinical research is carried out on animals, cells, in test tubes and on computers. Professor Erlinge does both, but mostly clinical research. Nearly all patients admitted to the clinic are included in a study of some kind, if they agree. Today’s patient is also asked for his consent even while being examined. He agrees without hesitation.
“Nine out of ten people are happy to take part. We have found that even those who are in a fairly poor state later remember being asked.”
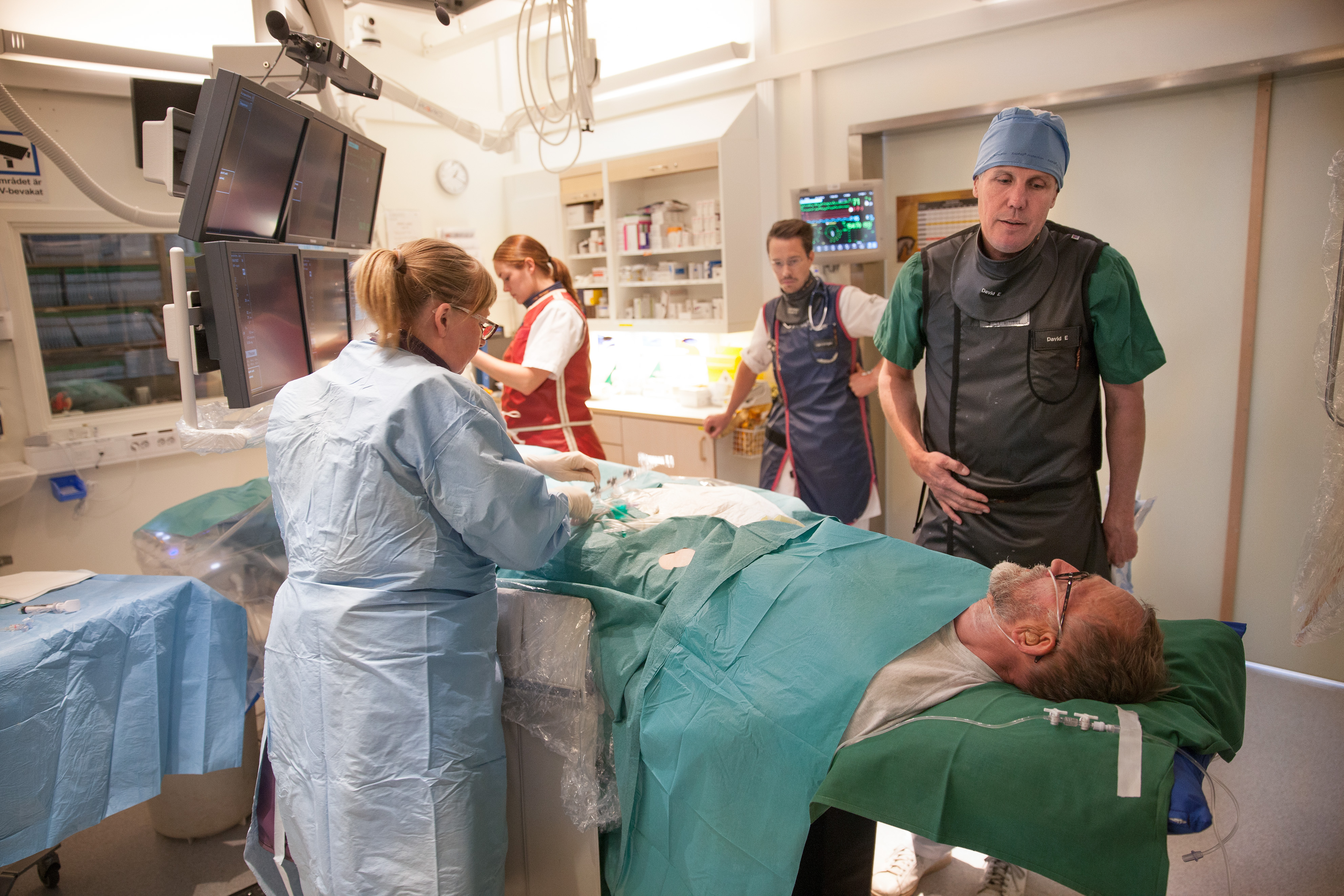
Fifty years ago nearly half of all those admitted to hospital with a cardiac arrest died. Today 95 percent survive, and many of them can go home the next day. Yet much remains to be done.
The first stage towards a heart attack is atherosclerosis, also known as hardening of the arteries. Fat is stored in the walls of the arteries, and forms plaque, which makes them narrower. This probably happens in all people, increasingly as we age. It is not necessarily dangerous, but if the plaque breaks up, it may form a clot, either in situ or where plaque fragments fasten somewhere else in the bloodstream.
Heart attacks are usually treated by removing the clot and opening the blocked artery, and by trying to prevent a new heart attack occurring. But the patient does not recover simply because the clot is removed. The damage can actually worsen in the short term. Professor Erlinge likens it to a starving person suddenly eating a Christmas dinner; it causes a shock to the system. More heart cells may die when blood flows to the “starved” areas.
But there seems to be a way of reducing the damage. The patient is cooled down for some hours during the treatment, to 33 degrees Celsius instead of the usual 37. This is what one of Erlinge’s research projects is about.
“I’ve never received a grant for more than three years before. As a Wallenberg Clinical Scholar, I will have a stable platform from which to plan for the longer term. This means I’ll be able to employ more doctoral students and statisticians, and conduct studies that take more than five years to complete.”
Today’s patient is not cooled down, however. He has a blocked artery opened and a stent inserted – a tiny metal tube that keeps the artery open. He is also given an anticoagulant. Another of Professor Erlinge’s projects aims at identifying the most effective anticoagulant. A third project is studying a new type of biodegradable stent. Current metal stents work well in many ways, but they make the arteries a little less flexible. This impedes blood flow, which increases the risk of more fat accumulating in the artery and forming a new clot.
The biodegradable stents being tested in Lund are made from lactic acid. They dissolve within one to two years, producing carbon dioxide and water, like mineral water. Research to date has shown the new stents to be neither less nor more effective than the old ones – but these findings relate solely to the first two years. Professor Erlinge thinks they will be found to reduce the risk of further heart attacks in the longer term, since the artery regains its natural flexibility.
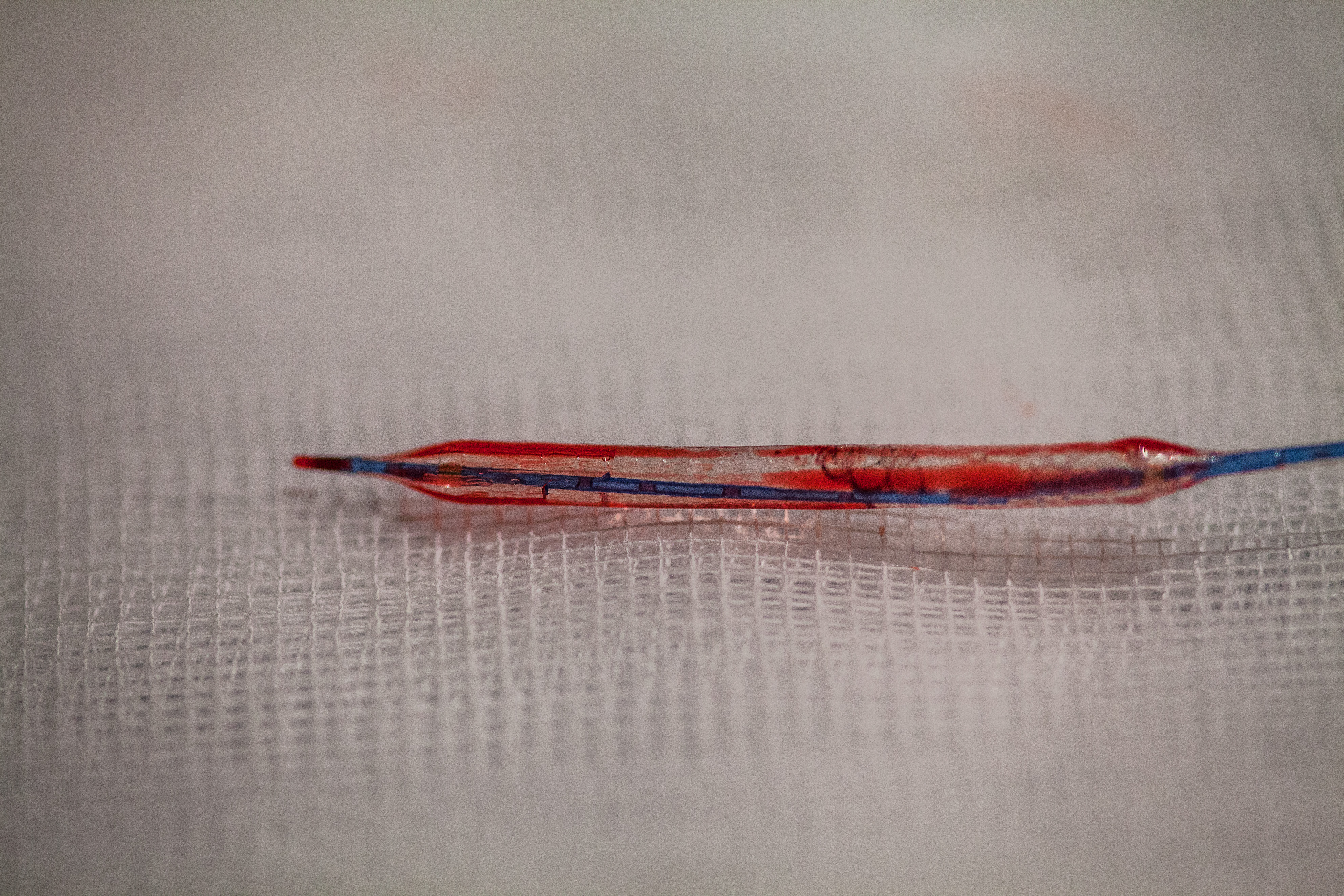
Biodegradable stents might also be an alternative for people who have not had a heart attack, but who are at risk. In one of Erlinge’s projects the coronary arteries of several hundred patients are being scanned using a technique called NIRS, which uses light close to the infrared spectrum. It appears to be able to show exactly which plaque in the artery is likely to break off. If the method is found to be reliable, it could be used on subjects with a high theoretical risk – smokers, overweight people, and the elderly – to reveal the actual risk they face.
“If the findings are really good, we will be able to decide who should receive preventive surgery.”
Even now it is possible to monitor certain parameters to estimate a patient’s risk. But this is not sufficiently reliable to be of practical use. In the future Professor Erlinge hopes to be able to offer a full range of better monitoring methods.
He is far from the only person conducting research at the clinic. His colleagues have become increasingly interested in research over the past fifteen years. For instance, Erlinge’s doctoral students have become specialists at the hospital, and have continued their research there.
“Although Swedish local authorities always say they support clinical research, it is not usually on their day-to-day agenda; it is seen more as an intrusion in the health care sector. But attitudes differ greatly from one clinic to another. At our clinic things are working out really well at the moment,” comments Professor Erlinge.
Text Lisa Kirsebom
Translation Maxwell Arding
Photo Magnus Bergström