Project Grant 2020
Human B cell development pathways
Principal investigator:
Professor Qiang Pan Hammarström
Co-investigators:
Petter Brodin
Lennart Hammarström
Hong Qian
Institution:
Karolinska Institutet
Grant in SEK:
SEK 39.2 million over five years
The body’s B cells were discovered in the late 1960s. However, we still know more about B cell development in mice than in humans.
“We want to gain a better molecular understanding of how B cells form and develop. We hope to answer questions such as how B cells differ from each other in different parts of the body, how they develop, and how they change during various diseases” says Qiang Pan Hammarström.
She is leading a project funded by Knut and Alice Wallenberg Foundation with the aim of mapping the development of our B cells.
Producing antibodies
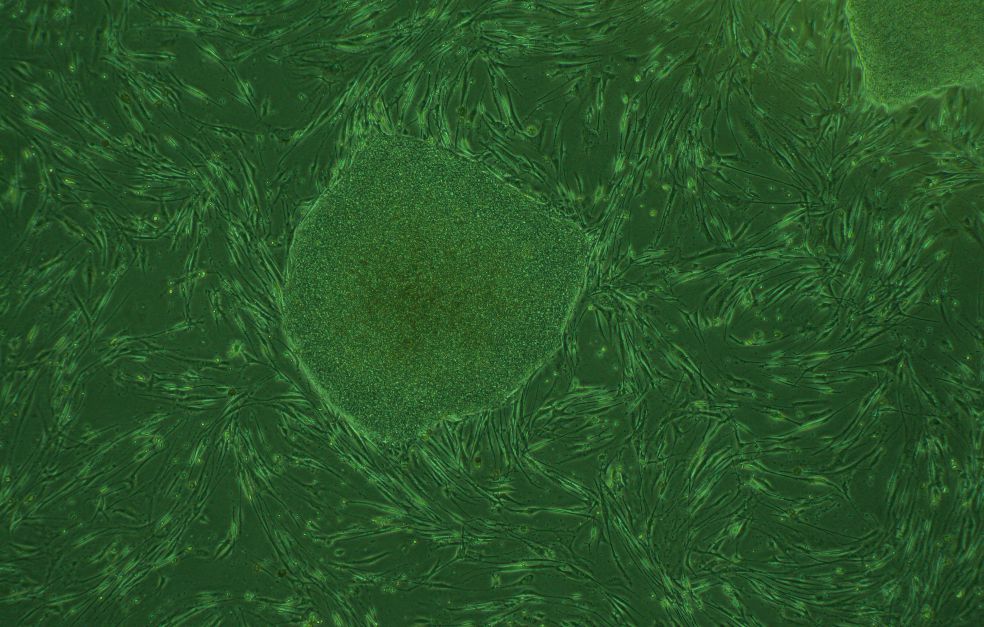
B cells form part of the adaptive immune response. They are called B cells because they are formed in the bone marrow. Tens of millions of new B cells are formed there every day, each with their own gene to create a unique antibody. The antibody’s task is to detect and attach itself to intruders, such as viruses. Each antibody clone is unique, which enables the immune system to identify a virtually infinite number of substances.
The B cells then patrol the blood and lymphatic system in search of intruders. If the cell does not find anything that can attach to the unique antibody, it will die within a few days. But if it comes across something that fits, an immune reaction begins, involving multiple immune cells. Aided by T cells, B cells begin to divide and produce large quantities of the specific antibodies.
The antibodies released by the B cells attach to the intruder and makes it easier for other immune cells to attack it. Some of the B cells do not develop into antibody factories, but rather they become B memory cells, which play a key role in future protection provided by the immune system. Those cells store a memory of the intruder so they can swiftly initiate an immune reaction should it return.
Pan Hammarström emphasizes that in understanding B cell development it is vital to make use of knowledge about human diseases.
“By understanding how different diseases relate to B cells, we can also gain a better understanding of immune system. We need to learn how to train the system to produce antibodies.”
Mapping the whole development chain
The project will be mapping the entire development chain from stem cell to the various forms of B cells. The research team is using single-cell sequencing to ascertain which genes are activated in each step. This will enable them to draw a development map of the cells. They are also using the CRISPR/Cas9 technology-based tool to carry out large-scale screening. Here, the aim is to see which transcription factors are particularly important in B cell development.
“Understanding each stage of development from stem cell to functional cells is a long process, requiring us to develop new models and systems in the lab,” Pan Hammarström says.
In mapping B cells in different tissues they are being assisted by the Center for Infectious Medicine (CIM) at Karolinska Institutet. The center has access of samples from different parts of the body from organ donors, including the lungs, intestines, bone marrow and the blood and lymphatic system. One of the problems, however, is that the number of B cells is so small compared with other immune cells.
“This caused us to underestimate the function of B cells in the immune system. But there is now a growing realization that they play a more important role in various conditions than we thought. Thus, I think we’ll find a large number of previously unknown subtypes of B cells in different parts of the body.”
A better understanding of immune-related diseases
The study also forms the basis for a comparison of B cells in healthy individuals with those suffering from various forms of immune-related diseases. These are diseases that either attack the body’s own tissues, i.e. autoimmune disorders, such as diabetes, celiac disease and rheumatism, or over response of our immune system, such as various allergic disorders, or with insufficient immune response, i.e. immunodeficiencies. Here, the team is being assisted by Lennart Hammarström’s research team, which has built up a bank of samples from individuals suffering from various immune-related disorders, including a number of rare genetic variants.
“The aim is first to create an atlas of the normal states of the various B cells. This can then be used to gain a better understanding of autoimmune diseases, as well as allergies, immune deficiency diseases and some types of blood cancer, in which B cells are involved to varying degrees,” says Pan Hammarström.
During the project the researchers will also be studying B cell development in new-born infants to see how various environmental factors such as delivery method, infections and vaccinations impact development.
Petter Brodin’s research will play a key role here. His team is conducting a project that is monitoring several hundred children from birth to about the age of three. They are monitoring and analyzing changes in the children’s immune cells, as well as proteins in their blood and the composition of their gut microbiome.
Pan Hammarström considers that the time is ripe for a project to map B cell development:
“Interest in our field has really exploded during the pandemic, so the timing of this project really is perfect.”
Text Magnus Trogen Pahlén
Translation Maxwell Arding
Photo Yating Wang, Qiang Pan Hammarström, Magnus Bergström